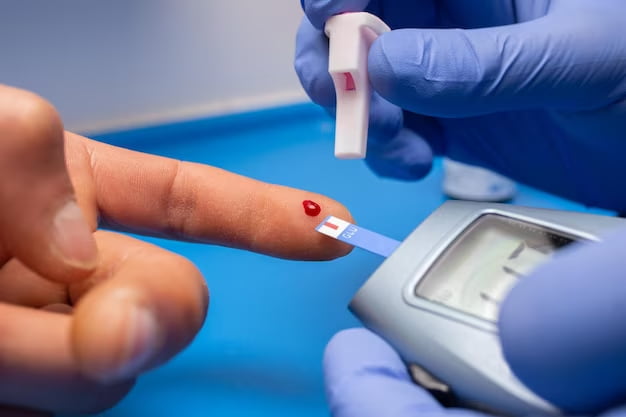
Metformin stands as a cornerstone in the realm of medications dedicated to the management of type 2 diabetes, commanding widespread usage. Garnering over 60 million prescriptions each year, this generic medication has solidified its popularity among both patients and healthcare practitioners. Beyond its ubiquity, a fundamental question arises: what mechanisms does metformin employ within the body to effectively regulate blood sugar levels? Delving into the intricacies of this diabetes drug is essential for patients seeking to harness its benefits with greater efficacy.
Metformin’s Effect on the Liver
One of the main ways that generic metformin helps regulate blood glucose levels is by decreasing glucose production in the liver. Normally, the liver releases stored glucose when blood sugar levels drop too low. This helps maintain normal blood sugar ranges. However, in diabetic patients, the liver may release too much glucose even when blood sugars are already high.
Metformin reduces excessive hepatic glucose production. It does this primarily by inhibiting gluconeogenesis, which is the process where the liver forms new glucose molecules from compounds like lactate, glycerol, and certain amino acids. With less glucose entering the bloodstream from the liver, metformin can help reduce fasting and post-meal blood sugar spikes.
Recent research has also shown that metformin may reduce glucose output from the liver by altering gut microbiome production of certain short-chain fatty acids that influence gluconeogenesis. This demonstrates that the drug’s mechanisms are not fully understood yet, with discoveries still emerging on how it regulates blood sugar balance.
Increasing Insulin Sensitivity
In addition to reducing glucose output from the liver, metformin also helps improve the body’s sensitivity to insulin. Insulin is the hormone that allows cells throughout the body to take up and utilize blood glucose for energy. In diabetes, cells become less responsive to insulin. This is known as insulin resistance.
By activating enzymes like AMPK, metformin makes cells more sensitive to insulin. This allows whatever insulin the body still produces to work more effectively. Improved insulin action means cells can take up glucose more readily. This further aids in lowering blood sugar levels.
Both insulin resistance and reduced insulin production contribute to diabetes development. The dual action of metformin addresses both defects by decreasing liver glucose output in the absence of insulin and enhancing the uptake of glucose into cells when insulin becomes available. By targeting both factors, metformin produces robust improvements in blood sugar control.
Other Beneficial Effects
Beyond its primary mechanisms of action, some research indicates metformin may have additional beneficial effects in diabetic patients. For example, studies show the drug may help with weight loss and cholesterol control – two important factors for diabetes management.
There is also evidence that metformin could play a protective role in diabetes complications. By keeping glucose levels within healthier ranges, the medication may help prevent or delay damage to the small blood vessels affected by chronically high sugars. This could potentially reduce the risk of problems like diabetic neuropathy, retinopathy, or cardiovascular damage.
Some scientists believe these extra benefits stem from metformin activating AMPK enzymes throughout the body. These proteins regulate cell metabolism and energy balance similar to insulin. By boosting AMPK activity, metformin produces positive impacts across many biological systems and organs beyond just blood sugar effects.
Understanding Proper Usage
While extremely helpful for controlling blood sugar, metformin does come with some potential side effects. The most common of these include digestive upsets like nausea, vomiting, diarrhoea and abdominal pain. To help minimize adverse effects, doctors recommend starting with low doses and taking the medication with food.
Extended-release tablet forms of generic metformin can also make the drug easier to tolerate. These tablets have a special coating allowing gradual absorption over hours rather than hitting the system all at once. This avoids sudden spikes in metformin levels that provoke stomach irritation.
As helpful as metformin can be, it does not replace other key pillars of diabetes care like nutrition therapy, exercise, and weight control. Lifestyle approaches combined with careful medication management offer the best results for gaining control over erratic blood sugars. Monitoring levels frequently with a glucometer allows patients to see how significantly small daily changes can impact their glucose trends.
Common Side Effects
In addition to gastrointestinal issues, there are some other potential side effects to be aware of with metformin use:
Lactic acidosis – The buildup of lactic acid in the blood is a rare but serious complication, mainly occurring in patients with kidney impairment. Symptoms include muscle pains, breathing difficulty, dizziness, and abdominal pain.
Vitamin B12 deficiency – Long-term use of metformin may result in vitamin B12 malabsorption, resulting in a deficiency if not properly supplemented. Symptoms can include anaemia, fatigue, constipation, appetite loss, and neuropathy.
Hypoglycemia – Although much less common than with other diabetes medicines, metformin may still increase hypoglycemia risk when combined with other drugs, alcohol use, skipped meals, or during intense exercise.
Being aware of potential adverse reactions allows for prompt reporting to your healthcare provider should any occur. Dose adjustments or additional nutritional supplementation may alleviate some side effects.
When Metformin Isn’t Enough
For some diabetic patients, metformin alone isn’t sufficient for achieving adequate blood sugar control. Over time the remaining insulin-producing beta cells in the pancreas can decline enough that metformin’s help improving insulin sensitivity isn’t impactful. In these cases, additional oral medications or injectable therapies like GLP1 drugs or insulin become necessary.
The American Diabetes Association recommends supplementing metformin with drugs like sulfonylureas, SGLT2 inhibitors, DPP4 inhibitors or thiazolidinediones if needed. Combination therapy leverages different mechanisms for reducing glucose levels. This allows patients to achieve tighter overall blood sugar management.
Conclusion: A Mainstay Medication for Diabetes Care
In conclusion, metformin is an invaluable medication for managing type 2 diabetes because it directly targets several physiological factors that influence blood glucose balance. From reducing hepatic glucose production to improving peripheral insulin sensitivity, metformin tackles erratic blood sugars on multiple fronts simultaneously.
While the drug does have some potential for side effects like digestive issues, proper dosage adjustments and the use of extended-release forms can often overcome these problems. When combined with lifestyle approaches emphasizing nutrition, activity levels, weight control, and frequent self-monitoring, metformin offers excellent blood sugar regulation pivotal for minimizing diabetes complications long-term. Understanding exactly how this staple medication exerts its helpful effects empowers patients to use it most effectively as part of a comprehensive diabetes treatment regimen.
Did you find this helpful? Check out our other helpful articles on our website.
Read Also
- The Best Low-Maintenance Landscaping Ideas for Ontario/BC HomeownersFor homeowners in Ontario and British Columbia, the yard is a sanctuary, but the maintenance required to keep it beautiful can often feel like a full-time job. Whether you are dealing with the humid, high-growth summers of Southern Ontario or the lush, moss-prone environments of the BC coast, the goal of modern landscaping has shifted:… Read more: The Best Low-Maintenance Landscaping Ideas for Ontario/BC Homeowners
- Understanding the Impacts of Metabolic Rates on General HealthYour metabolic rate plays a bigger role in your health than you might think. It controls how your body turns food into energy every single day. When metabolism is balanced, you may feel more active and focused. If it slows down or speeds up too much, problems can appear. It can affect weight, energy levels,… Read more: Understanding the Impacts of Metabolic Rates on General Health
- When to Take Your Child to the Pediatrician vs. Urgent Care: A Practical GuideFew parenting decisions feel more uncertain than the one made at 9 PM with a feverish toddler in your lap. Is this a wait-until-morning situation? A drive-to-urgent-care situation? A call-the-pediatrician’s-after-hours-line situation? Knowing the framework for these decisions cuts down on stress, reduces unnecessary trips, and makes sure your child gets the right care at the… Read more: When to Take Your Child to the Pediatrician vs. Urgent Care: A Practical Guide
- Well-Child Visits Explained: What Happens at Each Checkup and Why They MatterWell-child visits are one of the most useful — and most underestimated — tools in pediatric care. Many parents think of them as a vaccination delivery system, but they’re actually structured developmental checkpoints designed to catch issues early, track healthy growth, and give parents a regular opportunity to ask questions about everything from sleep to… Read more: Well-Child Visits Explained: What Happens at Each Checkup and Why They Matter
- Sprained Ankle vs. Fracture: How to Tell the Difference and What to Do NextA rolled ankle is one of the most common injuries in everyday life — a missed step on a curb, an awkward landing during a pickup game, a slip on uneven ground. Most of the time it’s a sprain that heals with rest. Sometimes it’s actually a fracture, and the two can be surprisingly hard… Read more: Sprained Ankle vs. Fracture: How to Tell the Difference and What to Do Next
- Plantar Fasciitis, Bunions, and Heel Pain: When Conservative Care Isn’t EnoughFoot pain is often dismissed as a nuisance — something to push through, stretch out, or ignore until it goes away. And in fairness, many cases do resolve with rest, better shoes, and basic stretching. But certain conditions can quietly worsen for months or years before patients seek help, by which point conservative options have… Read more: Plantar Fasciitis, Bunions, and Heel Pain: When Conservative Care Isn’t Enough
- Is Joint Replacement Right for You? Questions to Ask Before SurgeryJoint replacement is one of the most successful procedures in modern medicine — but it’s still major surgery, and it’s not the right answer for everyone. If chronic hip or knee pain has reached the point where you’re considering replacement, the questions you ask before scheduling can shape your outcome as much as the procedure… Read more: Is Joint Replacement Right for You? Questions to Ask Before Surgery
- When Knee Pain Won’t Go Away: Signs It’s Time to See an Orthopedic SpecialistKnee pain is one of those things many people try to ignore — until it starts limiting what they can do. A twinge after a workout is one thing; pain that lingers for weeks, swells without explanation, or makes the stairs feel like a mountain is something else entirely. Knowing when to stop self-treating and… Read more: When Knee Pain Won’t Go Away: Signs It’s Time to See an Orthopedic Specialist