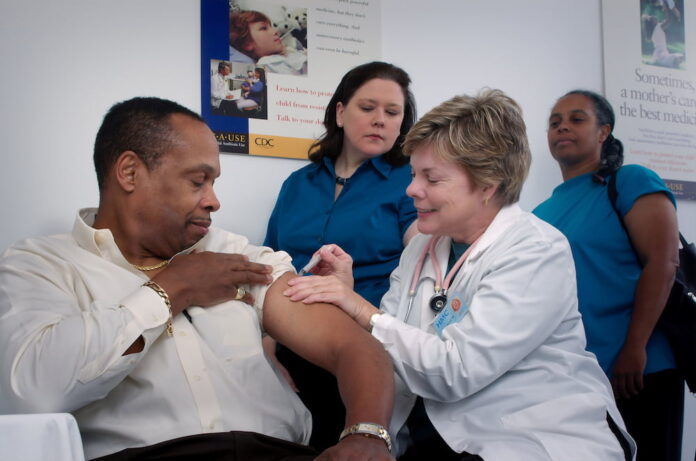
The healthcare system is essential to society, providing medical services and care for individuals. However, access to healthcare services and quality of care is not distributed equally among different social and economic groups. This disparity in healthcare results from various factors such as race, gender, income, and education and is a manifestation of systemic inequalities in society.
This article highlights essential things to remember about social justice in healthcare to promote equitable access to healthcare services and improve healthcare outcomes for all.
1. Addressing Health Disparities
Health disparities are the differences in health outcomes experienced by different groups of people. Its often due to social determinants of health such as poverty, racism, discrimination, and inadequate access to healthcare services.
Social justice in healthcare is key to addressing and promoting equity and health disparities. Ensuring that healthcare services are accessible, affordable, and of high quality for all individuals, regardless of their socioeconomic status or background, is the sole motive of social justice in healthcare.
According to Maryville University, addressing health disparities requires a multifaceted approach to addressing social determinants of health.
It promotes health literacy and implements policies and programs that support health equity. For example, Maryville University states that addressing poverty, inadequate housing, and food insecurity can improve overall health outcomes for individuals and communities. Additionally, promoting health literacy can empower individuals to take control of their health and make informed decisions about their healthcare needs.
Moreover, implementing policies and programs that promote health equity, such as Medicaid expansion, can improve access to healthcare services for low-income individuals and communities.
2. Cultural Competence
Cultural competence is the ability of healthcare providers to understand and respond to their patients’ unique cultural and linguistic needs. In addition, they must recognize that patients from different cultural and linguistic backgrounds may have unique healthcare needs, beliefs, and practices that may impact their healthcare experiences.
According to American Public Health Association, health disparities can be linked to more than 30% of the direct medical expenditures incurred by cultures like Asian Americans, U.S. Blacks, and Hispanics. Over four years, the 30% equates to more than $230 billion.
In addition, these populations frequently get worse even when they locate a source of treatment, resulting in increased medical expenses. It is because of unequal access to care and other resources that promote health.
Medical professionals must receive training and education on cultural competence to provide culturally competent care. This training should include information on cultural beliefs and practices, language access, and how to address cultural barriers in healthcare. Additionally, the providers must be aware of their own biases and assumptions and work to address them to provide equitable care to all patients.
3. Health Literacy
Health literacy refers to the ability of individuals to understand and access health information and services to make informed decisions about their health. Individuals with low health literacy may struggle to understand health information, leading to poor health outcomes and disparities in healthcare.
According to National Today, the ability to receive, absorb, and comprehend basic healthcare information required for making wise decisions is challenging for more than 40% of Americans.
If not given proper attention, healthcare illiteracy can substantially hamper attempts to provide healthcare. Thus, every year, October is recognized as Health Literacy Month to highlight its importance and awareness, which was started in 1999 by author Helen Osborne.
It was done to make healthcare information more widely available. Several camps and seminars are organized for medical professionals to explore how to raise health literacy worldwide.
Moreover, medical personnel must communicate health information clearly and understandably to promote health literacy. It includes using plain language, avoiding medical jargon, and providing visual aids to help patients understand complex health information. Additionally, they must ensure patients can access health information in their preferred language and format, such as audio or video.
4. Patient-Centered Care
Patient-centered care involves partnering with patients to ensure that their healthcare needs and preferences are at the forefront of their care. This approach to care acknowledges that patients have unique healthcare needs, beliefs, and preferences that must be considered to provide quality care.
Patient-centered care involves listening to patients, understanding their healthcare goals, and involving them in healthcare decision-making. Healthcare specialists must take the time to build relationships with patients and create a safe and trusting environment where patients feel comfortable sharing their healthcare concerns.
They can promote equitable access to healthcare services by involving patients in their healthcare decision-making. Patients from diverse backgrounds may have unique healthcare needs or cultural beliefs that impact their healthcare decision-making.
5. Collaborative Care
Collaborative care involves healthcare providers working together to provide coordinated and comprehensive patient care. This approach to care ensures that patients receive the right care, from the right provider, at the right time, regardless of their background or circumstances.
It coincides with the DEI (Diversity, Equity, and Inclusion) programs, which throughout the past 20 years, have been more important in the field of healthcare. According to Ernst & Young Global, DEI has been a starting point for health equity in recent years. As a result, healthcare providers now understand that worker equity results in patient equity and good medical outcomes.
About half (42%) of all surveyed firms, including nearly two-thirds (28%) of health systems and mental health institutions, prioritize DEI synergies in their overall strategy. It demonstrates that diversity and inclusion of employees are their top priorities regarding health equity.
Collaborative care involves these medical personnel providers from different disciplines working together to provide coordinated care. It includes primary care physicians, specialists, nurses, social workers, and other healthcare providers.
6. Advocacy and Community Engagement
Healthcare providers must engage with their local communities to better understand their healthcare needs and address healthcare disparities. It includes partnering with community organizations, advocacy groups, and policymakers to promote equitable access to healthcare services.
They must also advocate for policies and practices that promote equity in healthcare. It includes advocating for policies that address healthcare disparities, such as expanding access to healthcare services and reducing healthcare costs.
Additionally, Healthcare specialists can advocate for policies that address social determinants of health, such as affordable housing and access to healthy food.
Social Justice Must Prioritize Promoting Fairness in Healthcare
Promoting equity in healthcare is a critical component of social justice. Healthcare providers must recognize their patients’ unique healthcare needs and preferences and work to address healthcare disparities. It requires a patient-centered approach to care, cultural competence, and health literacy.
Additionally, these providers must engage with their local communities and advocate for policies promoting equitable healthcare access. Addressing healthcare disparities and promoting equitable access to healthcare services can improve health outcomes for all members of society. These could help work towards achieving social justice in healthcare.
Read Also
- Tax Optimization Strategies for Modern Healthcare ProfessionalsTax planning is important for healthcare workers today. Many people in this field work long hours and manage many costs. Because of this, saving money on taxes can help a lot over time. Good tax optimization strategies can help professionals keep more of what they earn. These methods can also support better financial goals in… Read more: Tax Optimization Strategies for Modern Healthcare Professionals
- The Hidden Liabilities of Hazardous Waste: Why Elite Environmental Management is Non-NegotiableLet’s be completely honest for a second. Running a commercial facility, a manufacturing plant, or a healthcare hub that handles dangerous materials is an absolute high-wire act. You aren’t just managing staff and worrying about profit margins; you are actively holding back potential disasters every single day. One tiny oversight—a leaking drum, a misread label,… Read more: The Hidden Liabilities of Hazardous Waste: Why Elite Environmental Management is Non-Negotiable
- Top Strategies for Implementing Remote Patient Monitoring SuccessfullyRemote patient monitoring is changing how care is delivered. It brings patients and providers closer, even from a distance. But success takes more than just devices and data. It requires clear planning, smart tools, and strong communication. Each step should focus on patient comfort and ease of use. Small improvements can lead to better outcomes… Read more: Top Strategies for Implementing Remote Patient Monitoring Successfully
- Navigating 21 CFR Part 11 in Modern Clinical LabsWhat ensures that digital records in clinical labs remain accurate, secure, and trustworthy? As laboratories rely more on digital systems, maintaining compliance with strict regulations becomes essential. One important standard is 21 CFR Part 11, which focuses on electronic records and signatures. It helps ensure that data is reliable and protected from misuse or errors.… Read more: Navigating 21 CFR Part 11 in Modern Clinical Labs
- Protecting Patient Privacy in the Digital Age: The Role of Secure Information HandlingHealthcare has undergone a major transformation in recent years. With the shift from paper records to digital systems, managing patient information has become both more efficient and more complex. Alongside these changes comes a growing need to protect sensitive data. This is where redaction software in healthcare plays an increasingly important role. Healthcare organizations handle… Read more: Protecting Patient Privacy in the Digital Age: The Role of Secure Information Handling